She’s 49. An attorney. Used to run half-marathons. Now she can barely drag herself through a 5K.
She’s gained 15 pounds despite eating less than she did in her thirties. She’s doing all the “right” things – counting calories, hitting the gym, cutting carbs. The scale won’t budge. Or it goes up.
Her previous doctor told her she was depressed and offered her an SSRI.
She’s not depressed. She’s not lazy. She’s not eating too much.
Her body has quietly switched to low-power mode without asking her permission.
If this sounds familiar, keep reading. Because what’s happening to you is not a character flaw – it’s a hormonal reality that most doctors were never trained to recognize, let alone treat.
Why “Eat Less, Move More” Fails Menopausal Women
Let me be direct: you can’t “lifestyle” your way out of the hormonal decline that comes with menopause. No amount of green tea, intermittent fasting, or extra spin classes will bring back the hormones lost when your ovaries run out of eggs.
This doesn’t mean lifestyle doesn’t matter – it absolutely does, and I’ll get to that. But if your foundation is crumbling and someone tells you to rearrange the furniture, you’re going to be frustrated. And that’s exactly what’s happening to millions of women right now.
Here’s why the standard weight loss advice catastrophically fails perimenopausal and menopausal women:
Your metabolic engine is losing its fuel. Estradiol – the primary estrogen your ovaries produced for decades – isn’t just a reproductive hormone. It’s a metabolic hormone. Estrogen receptors exist in your brain, muscles, fat cells, liver, and even inside your mitochondria (the energy-producing organelles in every cell). When estradiol drops, your entire metabolic system downshifts.
Your body is shifting where it stores fat. Before menopause, visceral fat (the dangerous kind around your organs) makes up about 5 – 8% of your total body fat. After menopause, that jumps to 15 – 20% – a three- to four-fold increase – and this happens independent of whether the number on the scale changes. You can weigh the same and be metabolically sicker.
Your muscles are shrinking. Estrogen supports muscle maintenance. As it drops, you lose lean mass – which means your basal metabolic rate drops. You’re burning fewer calories at rest, doing the same things you’ve always done.
Your mitochondria are under siege. Remove estrogen in animal models and mitochondrial oxidative stress increases by 150 – 200%. Brain mitochondrial function can drop by up to 30%. Your cells are literally producing less energy. This isn’t fatigue from being busy – it’s fatigue from your cellular power plants losing their maintenance crew.
Nothing is wrong with you. Your mitochondria just lost their maintenance crew.
Estrogen: The Metabolic Shield You Didn’t Know You Had
I think of estrogen as a shield – invisibly protecting your bones, brain, blood vessels, muscles, and metabolism for decades. The moment that shield dissolves, the enemy invades in full force.
Here’s what estrogen was doing for your metabolism that nobody talked about:
Maintaining insulin sensitivity. Estrogen helps your cells respond properly to insulin. When estrogen drops, insulin resistance develops – often years before your blood sugar looks abnormal on standard labs. Your fasting glucose might be fine while your body is pumping out dangerously high levels of insulin just to keep it there. This is called hyperinsulinemia, and it’s a metabolic time bomb hiding behind “normal” lab results.
Controlling fat distribution. Estrogen directs fat storage toward subcutaneous deposits (hips, thighs – metabolically relatively harmless) and away from visceral deposits (around organs – metabolically destructive). Lose estrogen, and fat migrates inward. Visceral fat doesn’t just sit there – it actively secretes inflammatory cytokines, worsens insulin resistance, and feeds a vicious cycle.
Powering your mitochondria directly. Estrogen receptor beta (ERβ) exists inside your mitochondria. It increases ATP production, promotes fatty acid oxidation, upregulates mitochondrial biogenesis (the creation of new mitochondria), and boosts antioxidant defenses. When estrogen leaves, your mitochondria lose the signal to burn fat efficiently. Your body’s ability to switch between fuel sources – what we call metabolic flexibility – degrades.
Before menopause, women actually oxidize fat more efficiently than men, burning a higher percentage of fat at every exertion level. This is an estrogen-mediated advantage. And it disappears.
The Hormonal Pile-On Nobody Mentions
Estrogen gets the headlines, but menopause weight gain is a multi-hormone problem. Here’s the full picture:
Cortisol: The Midsection Maker
Abnormal cortisol levels can negatively influence all of your other hormone pathways. During perimenopause, sleep deteriorates (thanks to declining progesterone and estrogen), stress response becomes dysregulated, and cortisol – your primary stress hormone – starts running the show.
High cortisol drives weight gain specifically around the midsection. It impairs glucose regulation, increases appetite, promotes visceral fat storage, and breaks down muscle tissue. And here’s the kicker: poor sleep raises cortisol, which disrupts other hormones, which worsens sleep. It’s a cascade, not a single domino.
Thyroid: The Silent Slowdown
Your thyroid controls your metabolic rate. And here’s something most doctors miss: the “normal” range for thyroid function is enormous. You can have a TSH of 4.0 – technically “normal” – and be profoundly hypothyroid.
Optimal thyroid ranges are much tighter than what most labs flag:
- TSH: 0.3 – 2.0 (not the standard 0.4 – 4.5)
- Free T3: 3.5 – 4.3 (the active thyroid hormone that actually runs your metabolism)
If your Free T3 is at the bottom of the range, you’re exhausted, your hair is falling out, and you can’t lose weight no matter what you do. But don’t worry – you’re technically “within normal limits.”
Normal is not optimal. (Sound familiar?)
Thyroid dysfunction also reduces metabolic activity throughout the digestive tract, contributing to the bloating that affects nearly 70% of perimenopausal and menopausal women – compared to 30% of the general population.
Progesterone: The Sleep Thief
When progesterone drops – and it’s usually the first hormone to decline, often years before your periods stop – you lose your body’s natural sleep aid and anxiety buffer. Oral micronized progesterone metabolizes into allopregnanolone, a neurosteroid that calms your nervous system through GABA receptor modulation.
Without it, sleep quality tanks. And without quality sleep, cortisol rises, growth hormone drops, insulin sensitivity worsens, and your body preferentially stores fat. Progesterone loss doesn’t directly cause weight gain, but it removes one of the key pillars holding your metabolic house together.
For more on how these hormonal shifts unfold, read my complete perimenopause guide.
Your Gut Is Part of This Too
There’s a specialized community of gut bacteria called the estrobolome that metabolizes and regulates estrogen in your body. These bacteria produce an enzyme (β-glucuronidase) that controls how much estrogen gets recirculated versus excreted.
When menopause disrupts your hormonal environment, your gut microbiome shifts too. Beneficial bacteria – particularly Lactobacillus and Bifidobacterium – decline. Inflammatory species multiply. Intestinal permeability increases, allowing inflammation to leak into your system.
The result is a feedback loop: hormonal chaos disrupts your gut microbiome → dysbiosis increases intestinal permeability → visceral fat accumulates → inflammation destabilizes hormones further. A 2025 study of over 70,000 women found that gut microbial composition could actually predict the severity of menopause symptoms.
Bacteria specifically linked to weight management – like Akkermansia muciniphila and Christensenella minuta – decline after menopause, while the Firmicutes-to-Bacteroidetes ratio shifts in favor of weight gain.
This is why addressing gut health in midlife matters – it’s not separate from your hormone story. It’s part of it.
Hormone Optimization Is a Metabolic Intervention
Here’s what I need you to understand: hormone replacement therapy isn’t just about hot flashes. When we optimize estrogen, progesterone, and testosterone, we are intervening in a metabolic crisis.
The data on HRT and metabolic health:
- Better blood glucose regulation and reduced diabetes risk
- Reduced visceral fat – the dangerous kind
- Reduced blood pressure
- Improved lipid profiles – lower LDL, lower ApoB, lower Lp(a), higher HDL
- Cardiovascular protection – the Nurses’ Health Study (120,000 women, 20 years) showed a 40% reduction in cardiovascular disease when estrogen was started near menopause
And testosterone – the hormone almost no one offers women – directly builds muscle and reduces body fat. A double-blind, placebo-controlled trial showed testosterone therapy improved muscle power, stair-climbing ability, and lean body mass in a dose-dependent manner.
When we replace estrogen in the right form, at the right dose, at the right time, we’re not just treating symptoms. We’re restoring the mitochondrial maintenance program your body relied on for decades. We’re giving your cells back their fuel source, their fat-burning instructions, and their antioxidant defenses.
For the full breakdown of hormone therapy options, read my complete guide to HRT for women.
The Lifestyle Levers That Actually Work (Alongside Hormones)
Lifestyle interventions alone won’t fix a hormone deficit. But lifestyle interventions with hormone optimization? That’s where the magic happens. Here’s what moves the needle:
Resistance Training (Non-Negotiable)
Every strength session issues a construction order for new mitochondria. More muscle mass means more mitochondrial density, which means a higher metabolic rate. This is your single most important exercise modality in midlife – more important than cardio.
Resistance training also directly stimulates bone building (critical, since bone density starts declining before periods stop), improves insulin sensitivity, and increases your capacity to burn fat at rest.
Zone 2 Cardio
This is the conversational-pace cardio – where you can talk but it’s slightly uncomfortable. Zone 2 trains your mitochondria to burn fat efficiently. It builds the metabolic flexibility that estrogen used to support automatically. Aim for 150 – 180 minutes per week.
Protein
Mitochondrial enzymes and repair machinery require amino acids. You can’t build new mitochondria or maintain existing ones without sufficient protein. Most midlife women are dramatically under-eating protein. Aim for 1 gram per pound of ideal body weight – and front-load it earlier in the day.
Sleep
Sleep triggers mitophagy – the cleanup process that removes damaged mitochondria and recycles their parts into new ones. No sleep means no cleanup, which means accumulating mitochondrial debris. Progesterone replacement often dramatically improves sleep quality, which cascades into better cortisol regulation, better insulin sensitivity, and better body composition.
Creatine
Yes, creatine. It’s not just for bodybuilders. Creatine (3 – 5g daily) enhances muscle power and strength, especially when combined with resistance training, and may help maintain lean body mass during weight management efforts.
The GLP-1 Question
I can’t write about menopause weight management in 2026 without addressing GLP-1 receptor agonists – drugs like semaglutide (Ozempic/Wegovy) and tirzepatide (Mounjaro/Zepbound).
These medications have revolutionized the treatment of obesity and diabetes. They enhance insulin secretion, suppress appetite, slow gastric emptying, and have cardiovascular benefits beyond weight loss. GLP-1 receptors exist on immune cells, neurons, endothelial cells, and fat tissue – suggesting effects that go far beyond appetite suppression.
I’ve written about microdosing GLP-1s – using lower doses for metabolic optimization rather than aggressive weight loss. Some patients show improvements in inflammatory markers and metabolic function without losing a pound, suggesting direct anti-inflammatory effects.
But here’s my position: GLP-1s are a tool, not a foundation. If your hormones aren’t optimized, you’re treating downstream effects while ignoring the upstream cause. Optimize hormones first. Layer in lifestyle. Then consider GLP-1s if additional metabolic support is needed.
And for those who want a gentler approach: tributyrin, a short-chain fatty acid supplement, activates your body’s own GLP-1 production naturally. Some call it “nature’s Ozempic.” It’s one of the supplements I recommend for perimenopausal women alongside dihydroberberine for insulin sensitivity.
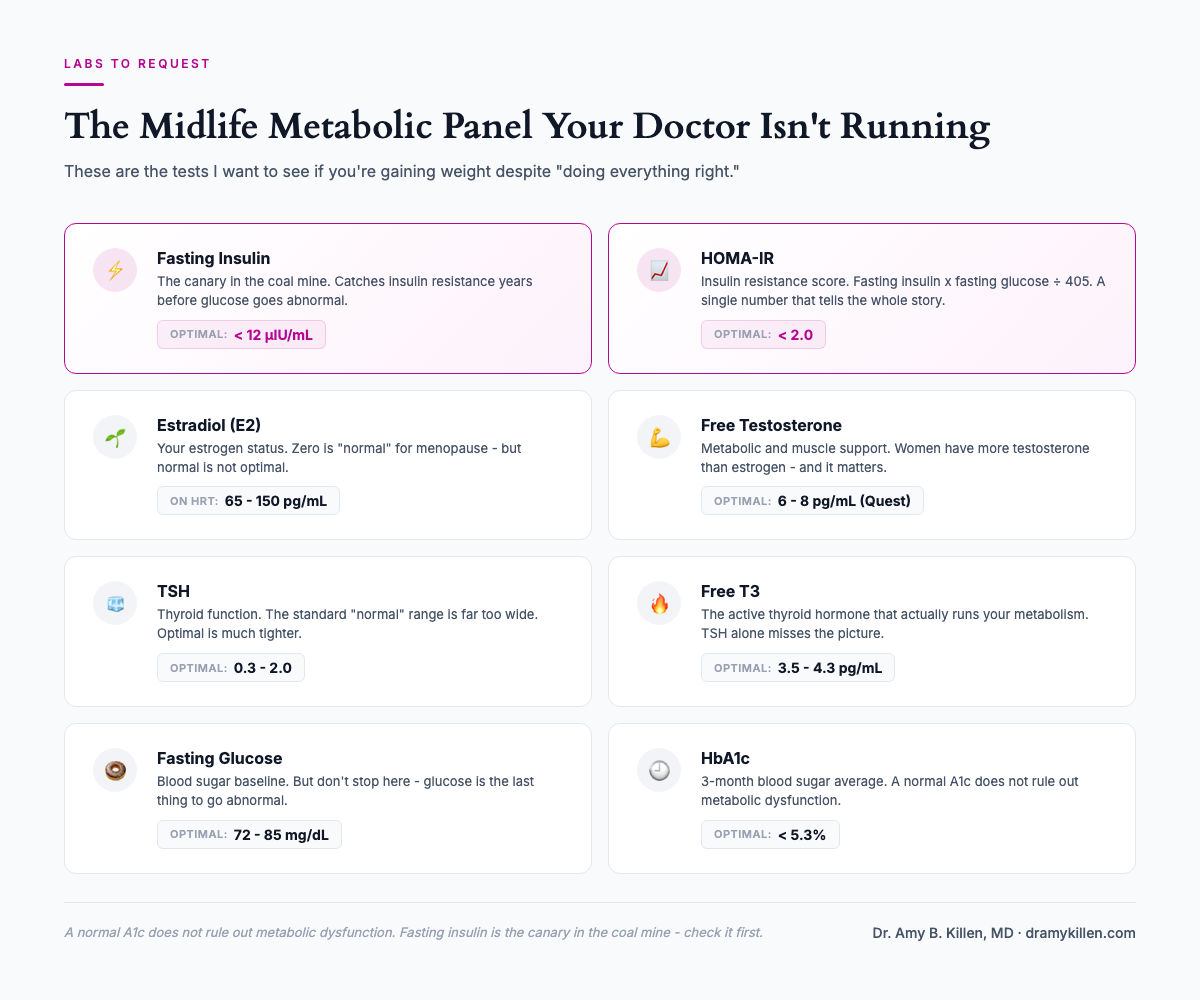
What to Track and What to Ask Your Doctor
If you’re gaining weight in midlife despite “doing everything right,” here’s what I’d want to see on your labs:
| Test | What It Tells You | Optimal Range |
|---|---|---|
| Fasting insulin | Insulin resistance (before glucose goes abnormal) | <12 μIU/mL |
| HOMA-IR | Insulin resistance score (fasting insulin × fasting glucose ÷ 405) | <2.0 |
| Estradiol (E2) | Estrogen status | 65 – 150 pg/mL on HRT |
| Free testosterone | Metabolic and muscle support | Quest: 6 – 8 pg/mL; LabCorp: 3 – 4 pg/mL |
| TSH | Thyroid function | 0.3 – 2.0 (not the standard 0.4 – 4.5) |
| Free T3 | Active thyroid hormone | 3.5 – 4.3 pg/mL |
| Fasting glucose | Blood sugar | 72 – 85 mg/dL |
| HbA1c | 3-month blood sugar average | <5.3% |
Critical point: a normal A1c does not rule out metabolic dysfunction. You can have significant insulin resistance with a perfect A1c if your body is compensating through hyperinsulinemia. Fasting insulin is the canary in the coal mine.
If your doctor isn’t familiar with these optimal ranges – or doesn’t test fasting insulin – you may need a provider who specializes in hormone optimization. I built the HOT Provider Course specifically to train these providers, and Humanaut Health clinics practice this approach from day one.
The Bottom Line
Menopause weight gain is not your fault. It’s not a failure of willpower or discipline. It’s the predictable metabolic consequence of losing the hormones that ran your metabolism for decades.
The solution isn’t another diet. It’s not another SSRI. It’s understanding what’s actually happening – at the hormonal, mitochondrial, and metabolic level – and addressing it directly.
Optimize your hormones. Build muscle. Feed your mitochondria. Fix your sleep. And stop blaming yourself for a problem that was never about willpower.
Welcome to your Queen Phase. It’s time to take your metabolism back.
NMN and Ca-AKG support mitochondrial function and metabolic health – both are in the HOP Box. Amy built HOP Box because she couldn’t find a supplement subscription that had clinical doses of the ingredients that actually matter for midlife women.
Dr. Amy Killen is a board-certified physician specializing in hormone optimization and regenerative medicine. She is the CMO and co-founder of Humanaut Health, founder of HOP, and creator of the HOT Provider Course. Follow her on Instagram and Substack for more.
References
- Rettberg JR, Yao J, Brinton RD. Estrogen: a master regulator of bioenergetic systems in the brain and body. Front Neuroendocrinol. 2014;35(1):8-30.
- Nilsen J, Irwin RW, Gallaher TK, Brinton RD. Estradiol in vivo regulation of brain mitochondrial proteome. J Neurosci. 2007;27(51):14069-14077.
- Mauvais-Jarvis F, Clegg DJ, Hevener AL. The role of estrogens in control of energy balance and glucose homeostasis. Endocr Rev. 2013;34(3):309-338.
- Gupte AA, Pownall HJ, Hamilton DJ. Estrogen: an emerging regulator of insulin action and mitochondrial function. J Diabetes Res. 2015;2015:916585.
- Davis SR, et al. Testosterone for women: the clinical biochemistry of detection and treatment. Clin Biochem Rev. 2016;37(4):167-184.
- Manson JE, et al. Menopausal hormone therapy and long-term all-cause and cause-specific mortality. JAMA. 2017;318(10):927-938.
- Stampfer MJ, et al. Postmenopausal estrogen therapy and cardiovascular disease: ten-year follow-up from the Nurses’ Health Study. N Engl J Med. 1991;325(11):756-762.
- Baker JM, Al-Nakkash L, Herbst-Kralovetz MM. Estrogen-gut microbiome axis: physiological and clinical implications. Maturitas. 2017;103:45-53.
- Lovejoy JC, Champagne CM, de Jonge L, et al. Increased visceral fat and decreased energy expenditure during the menopausal transition. Int J Obes. 2008;32(6):949-958.
- Hodis HN. Menopausal hormone therapy and cardiovascular disease prevention. Climacteric. 2023;26(4):309-316.
Are you a medical provider? Learn to prescribe hormone optimization therapy with the frameworks, protocols, and confidence you didn’t get in training.
Get Dr. Amy Killen’s Newsletter
Hormones, longevity, and regenerative medicine — straight talk from a physician who actually prescribes it. Free, weekly-ish, no spam.









